Mobitz Type I
What Is It, Causes, Signs and Symptoms, Diagnosis, Treatment, and More
What is Mobitz type I?
Mobitz type I is a type of 2nd degree AV block, which refers to an irregular cardiac rhythm (arrhythmia), that reflects a conduction block in the electrical conduction system of the heart.
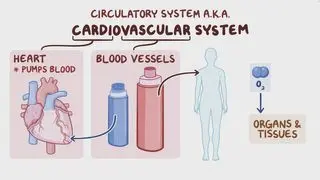
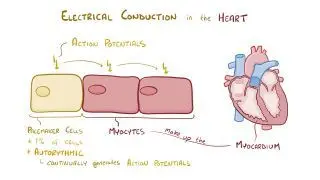
The heart is a muscular organ composed of four chambers: two upper chambers—the right and left atria—, and two lower chambers— the right and left ventricles. The chambers of the heart are wired with an electrical conduction system much like the electrical system of a house. This system consists of the sinus node, the atrioventricular (AV) node, the bundle of His, the right and left bundle branches, and Purkinje fibers. These conduction pathways are a network of highly specialized cells that generate and conduct electrical impulses, allowing the heart to contract rhythmically and pump out blood with each heartbeat.
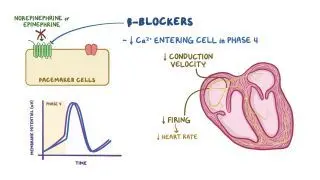
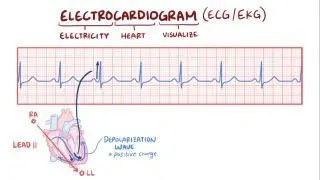
The heart’s electrical activity can be monitored with an electrocardiogram (ECG), which uses several electrodes (leads) to register the heart’s electrical activity from different angles. Electrical signals are first fired at the sinus node, where they then travel through the walls of the atria, triggering atrial contraction and the consequent movement of blood into the ventricles. During atrial contraction, the ECG will show a small deflection of the basal line, called the “P wave”. Next, the electrical signal is conducted through the AV node and then to the ventricles through the bundle of His and Purkinje fibers. This triggers ventricular contraction which pushes blood out of the heart and into circulation, resulting in a larger set of waves on the ECG that form the “QRS complex”. The interval between the onset of the P wave and QRS complex is known as the “PR interval”, and reflects the typical slowed conduction through the AV node. After the QRS complex, there’s another deflection called the “T wave”, which corresponds to the relaxation of the ventricles.
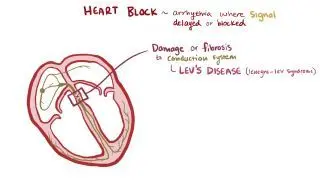
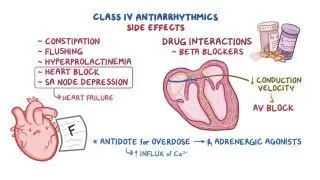
An atrioventricular block (AV block), also known as a heart block, occurs when an atrial impulse gets delayed or completely blocked at some point along the electrical conduction system of the heart. There are three degrees of AV block, according to the location and severity of the nodal block. A 1st degree AV block is not technically a block, but rather a delay in the conduction of atrial impulses to the ventricles, which results in an extended PR interval. Meanwhile, a 2nd degree AV block occurs when some of the atrial impulses are fully conducted to the ventricles, whereas others are blocked along the way. Blocked atrial impulses can be seen as a P wave that is not followed by a QRS complex, resulting in an irregular cardiac rhythm. Finally, a 3rd degree AV block occurs when none of the atrial impulses are conducted, leaving the atria and ventricles completely disconnected from one another. On the ECG, it can be detected by a total lack of correlation between the P waves and QRS complexes.
Are Wenckebach and Mobitz type I the same thing?
What is the difference between Mobitz I and Mobitz II?
Mobitz I and Mobitz II also differ in the severity of the conduction block. Mobitz I is a benign rhythm that generally reflects a block at the AV node, and typically results in a good prognosis. On the other hand, Mobitz II reflects a block after the AV node, either at the bundle of His or its branches, and often results in a poorer prognosis, as it has a higher risk of progressing to a 3rd degree AV block.