Rupture of diaphragm: Nursing
Notes
| RUPTURE OF DIAPHRAGM | ||
| KEY POINTS | NOTES | |
| DEFINITION |
| |
| PHYSIOLOGY |
| |
| CAUSES AND RISK FACTORS |
| |
| PATHOPHYSIOLOGY |
| |
| SIGNS AND SYMPTOMS |
| |
| DIAGNOSIS |
| |
| TREATMENT |
| |
| MANAGEMENT OF CARE |
| |
| PATIENT AND FAMILY TEACHING |
| |
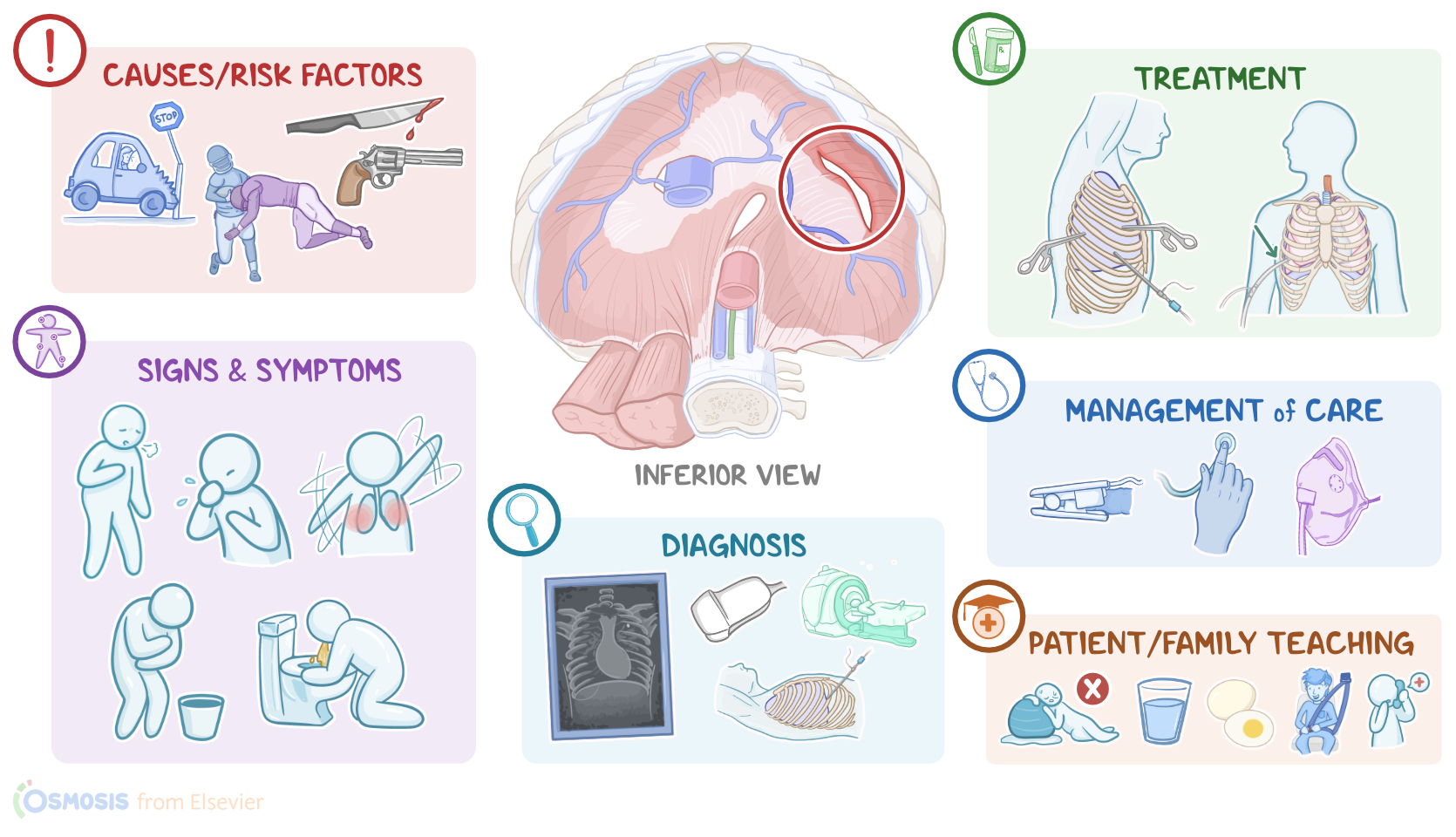
Transcript
Diaphragm rupture refers to tears of the diaphragm, mostly caused by blunt or penetrating trauma to the abdomen.
Now, let’s quickly recap the anatomy and physiology of the diaphragm, which is a dome-shaped sheet of skeletal muscle that divides the thoracic cavity from the abdominal cavity. It curves superiorly into right and left domes, or hemidiaphragms, with the liver lying just beneath the right dome. It has a mobile, central portion known as the central tendon and a peripheral muscular portion that is fixed to the bones, cartilages, and ligaments of the thoracic cage.
Now, the diaphragm is the chief muscle for inspiration; meaning that when it contracts, it helps us breathe in. During contraction, the central portion of the diaphragm depresses, increasing the volume of the thoracic cavity, which, in turn, increases the volume in the lungs. This makes the intrapulmonary pressure fall below the atmospheric pressure, creating a partial vacuum that allows fresh air to be sucked in! The diaphragm also helps with circulation. During contraction, the increased intra-abdominal pressure and decreased intrathoracic pressure help with the venous return of blood towards the heart through the inferior vena cava.
Now, the most common cause of diaphragm rupture is penetrating injury to the thorax or the abdomen, like a knife or gunshot wound, which can pierce through the diaphragm.
Less commonly, diaphragm rupture can be caused by blunt abdominal trauma, such as a motor vehicle crash, which causes a sudden increase in intra-abdominal pressure, causing the diaphragm to rupture. This rupture is far more common on the left hemidiaphragm compared to the right hemidiaphragm, which is protected by the liver.
Okay, let’s look at what happens when there’s a tear in the diaphragm. First, abdominal organs, like the stomach or bowel, may herniate or pass through the diaphragm tear. These abdominal organs increase the intrathoracic pressure and push against the lung, which decreases respiratory function. They can also compress blood vessels supplying the lungs, causing pulmonary hypertension. Now an interesting fact is that herniation is mainly a complication of larger diaphragm tears, which are most often caused by blunt abdominal trauma.
However, incarceration happens if the stomach or bowel herniates through a smaller diaphragm tear, which is when the herniated structure gets stuck and can’t go back into the abdominal cavity. In severe cases, the muscle of the diaphragm may strangulate or squeeze around the incarcerated organ, cutting off its blood supply, and leading to ischemia, and perforation or rupture of the stomach or bowel.
In some cases, diaphragm rupture can also be associated with hemothorax, or bleeding into the pleural space, as well as tension pneumothorax, where there’s a one way valve that lets air into the pleural space but prevents it from leaving, so it accumulates quickly in the pleural space, causing it to balloon up. Eventually, it’ll start compressing the other organs in the mediastinum like the heart, leading to cardiovascular impairment, which is fatal if left untreated.
Clients with diaphragm rupture are often asymptomatic, especially if it’s due to a penetrating injury. Their chief complaint will be the injury that leads to rupture and its associated symptoms. Injury to the diaphragm impedes normal breathing and the client can present with shortness of breath, cough, chest pain, and respiratory distress, which presents as short, shallow, and rapid breathing, as well as decreased SpO2. In the case of blunt trauma, these symptoms can be caused by a mix of impaired diaphragm function as well as damage to organs in the chest cavity such as the heart and lungs. Clients may also experience gastrointestinal symptoms, such as nausea and vomiting.
Inspection of the thorax shows asymmetrical chest expansion. During auscultation, there are reduced or absent breath sounds on the affected side. With bowel herniation, bowel sounds might also be heard over the chest. On percussion, there’s often dullness over the affected area, and on palpation, there might be decreased fremitus.
The diagnosis of diaphragm ruptures starts with the client’s history, and physical assessment, followed by a chest X-ray, which shows an elevated hemidiaphragm on one side. If parts of the GI tract have herniated through the tear, that could present with air bubbles in the thoracic cavity. However, other conditions might cause similar bubbles, so an insertion of a nasogastric, or NG, tube can help make the diagnosis. That’s because if the NG tube shows up in the chest cavity after insertion, it means a part of the GI tract has herniated. Additional imaging tests, such as ultrasound and CT scan might be also useful. In cases of small tears that can’t be visualized by imaging tests, thoracoscopy or laparoscopy might be required.
The treatment of diaphragm rupture depends on its severity. Small tears in the right hemidiaphragm generally only need close monitoring. In contrast, larger tears typically require laparoscopic surgery, during which the herniated abdominal structure is pushed back to the abdominal cavity and the diaphragm tear is stitched shut. After the procedure, a chest tube is often placed into the thoracic cavity to drain fluids or air, which helps with the reinflation of the lungs.
Alright, now let’s move on to talking about the management of care for a client diagnosed with diaphragm rupture. Your priority goals of care are to maintain adequate oxygenation and ventilation.
Key Takeaways
Rupture of the diaphragm is a condition in which the diaphragm, a sheet of muscle that separates the chest and abdominal cavities, tears or breaks. It is usually caused by penetrating trauma or blunt abdominal trauma, and risk factors include sustaining injuries such as gunshot wounds, stab wounds, falls, and being involved in a motor vehicle crash.
A ruptured diaphragm can cause serious medical complications and even death if it is not treated quickly. People with a ruptured diaphragm can present with shortness of breath, cough, chest pain, and respiratory distress, which presents as short, shallow, and rapid breathing, as well as decreased SpO2, but these manifestations may be masked by other injuries the client sustained.
Diagnosis is made based on history, physical exam, and imaging findings on chest X-ray as well as other imaging methods such as ultrasound or chest CT. Treatment depends on the severity, with small tears only requiring monitoring and large tears requiring surgical repair and chest tubes post-operatively. Management of care focuses on maintaining adequate oxygenation and ventilation.